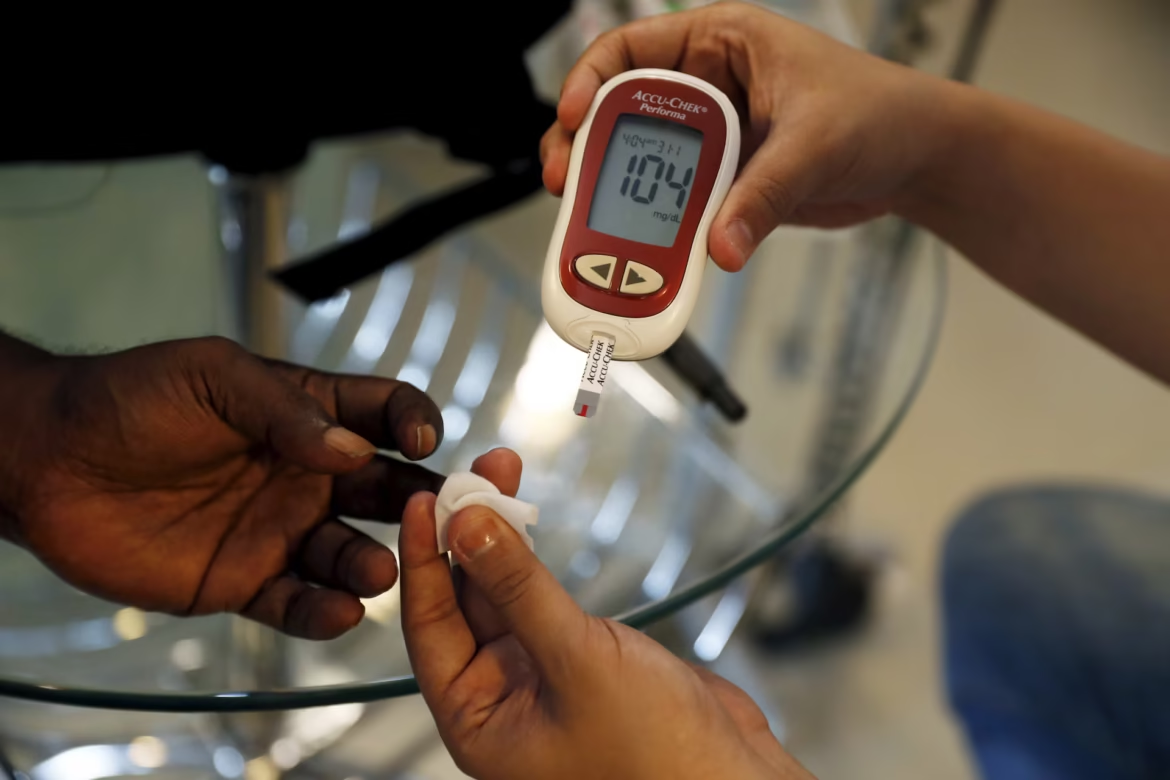
People who live high in the mountains have long puzzled scientists. Despite thinner air and lower oxygen levels, rates of diabetes in these populations tend to be lower than among people living at sea level. Now, researchers believe they have uncovered a biological explanation — one that could reshape how diabetes is treated in the future.
In a study published in the journal Cell Metabolism, scientists reported that under low-oxygen conditions, red blood cells undergo a remarkable shift. Instead of simply transporting oxygen, they begin absorbing more glucose from the bloodstream, effectively acting as “glucose sponges.”
Red Blood Cells: More Than Oxygen Carriers
At high altitudes, the body adapts to limited oxygen in several ways. One key adjustment is producing more red blood cells to improve oxygen delivery. But researchers discovered something even more intriguing: each of these cells also increases its glucose uptake.
This extra glucose provides red blood cells with the energy they need to efficiently circulate oxygen throughout the body. As a side effect, however, blood sugar levels drop — reducing the risk of developing diabetes.
Earlier experiments in mice revealed that animals breathing low-oxygen air experienced dramatically reduced blood glucose levels. After eating, their bodies cleared sugar from the bloodstream almost immediately. Scientists initially examined major organs such as the liver, brain, and muscles, expecting to find the explanation there. Instead, the answer lay within the blood itself.
The research team ultimately identified red blood cells as the true “glucose sink” — the primary site where excess glucose was being absorbed and used.
A Potential Game-Changer for Diabetes Treatment
Building on this discovery, researchers developed a drug called HypoxyStat. The medication mimics low-oxygen conditions by causing hemoglobin to hold onto oxygen more tightly, limiting its release to tissues and triggering similar metabolic adaptations.
In diabetic mice, HypoxyStat completely normalized high blood sugar levels. According to the researchers, the drug outperformed some existing treatments in experimental settings.
Rather than targeting insulin or organs traditionally associated with glucose control, this approach recruits red blood cells to remove excess sugar from circulation. It represents a fundamentally new way of thinking about diabetes therapy — one that may open promising avenues for future treatment.
Brain Cells Play a Surprising Role in Muscle Endurance
While muscles are often credited for improved stamina, new research suggests the brain plays a critical — and previously underappreciated — role in building endurance.
In findings published in Neuron, scientists studying mice discovered that specific brain cells are essential for improving stamina during exercise.
The Brain-Muscle Connection
Researchers focused on a group of neurons located in the hypothalamus that produce a protein known as steroidogenic factor-1 (SF1). These neurons became highly active for about an hour after mice completed treadmill sessions.
Over weeks of training, more SF1 neurons were activated following exercise. Additionally, connections between these neurons strengthened and multiplied. Mice that exercised regularly had nearly twice as many neural connections in this region compared to sedentary mice.
The most striking finding came when scientists temporarily silenced these neurons for just 15 minutes after each workout. Despite running as hard as before, the mice stopped gaining endurance. Their performance even declined over time.
Conversely, when researchers artificially stimulated the SF1 neurons for an hour after exercise, the mice achieved greater stamina and higher maximum speeds than usual.
Rethinking Exercise Science
These findings challenge long-held assumptions that endurance gains stem solely from muscle adaptation. Instead, they suggest that post-exercise brain activity is crucial for translating physical effort into lasting performance improvements.
The implications are significant. If scientists can learn how to safely activate or mimic these neural circuits, it may one day enhance the benefits of moderate exercise — particularly for older adults or individuals with limited mobility who cannot engage in intense physical training.
A New Era of Metabolic and Performance Research
Together, these studies highlight a broader shift in biomedical research. Whether examining how red blood cells regulate glucose under low oxygen or how brain circuits shape muscle endurance, scientists are uncovering hidden systems that influence health in unexpected ways.
As researchers continue exploring these pathways, the potential for innovative therapies — from novel diabetes treatments to enhanced exercise benefits — appears more promising than ever.